
Management starts with discontinuing feedings, fluid resuscitation with normal saline and nasogastric tube decompression. The more distal the obstruction, the more loops appear distended with air- fluid levels. Instead, jejunal atresia might have a “triple-bubble” appearance, in which the third bubble is caused by distention of the proximal jejunum. This is the result of the distended stomach and duodenum being separated by the muscular pyloric valve. In this situation, a baby may have bilious vomiting soon after birth.ĭiagnosis is usually made with ultrasound or with an abdominal X-ray in an upright position, in which duodenal atresia will appear as a “double-bubble”, with no air in the distal bowel. Since the fetus is less able to swallow amniotic fluid, more of it sticks around in the amniotic sac, which is called polyhydramnios and is detected on a prenatal ultrasound. Now, signs of atresia are usually present long before birth. Non- duodenal atresias, on the other hand, like those affecting the jejunum, ileum, or even the colon, are thought to be caused by lack of blood flow, to the developing gut. Next, there’s intestinal atresia or stenosis, which is when some portion of the intestine is absent or narrowed.ĭuodenal atresia is typically a result of a failure of recanalization of the duodenum in utero and it’s commonly associated with trisomy 21, or Down syndrome. 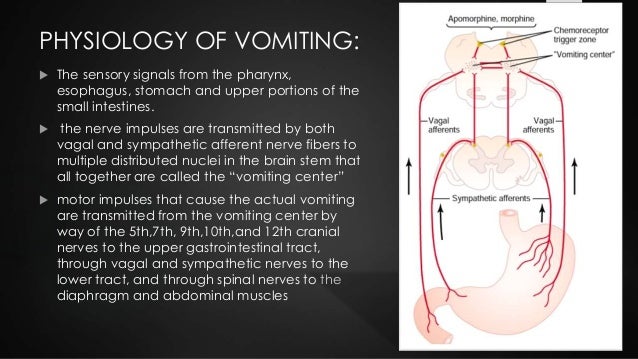
Emergency surgery, known as a Ladd procedure, should be performed, which is where necrotic bowel is resected and reoriented within the abdominal cavity. Management starts with discontinuing feedings, fluid resuscitation with normal saline, nasogastric tube decompression, and broad spectrum IV antibiotics, like vancomycin or 4th generation cephalosporins, to treat sepsis. That’s followed by an upper GI contrast series, which shows a corkscrew-like or spiral shaped duodenum in the right lower quadrant instead of the left upper quadrant. In fact, bowel infarction can also damage the intestinal wall and allow the bacteria in the gut to move into the body, which can cause sepsis.ĭiagnosis is usually made with ultrasound or with an abdominal X-ray in an upright position, which will show distended loops of bowel with air-fluid levels. This causes symptoms like acute, bilious vomiting, accompanied with abdominal distention and bloody diarrhea. 
In intestinal malrotation with volvulus, there’s twisting of the mesentery around the superior mesenteric artery leading to intestinal obstruction, infarction, and necrosis. This may be caused by intestinal malrotation with volvulus, atresia or stenosis of the lower duodenum or intestines, or by Hirschprung’s disease. Now, if the obstruction is after the junction of the duodenum with the bile ducts at the ampulla of Vater, then the vomiting is bilious. Pathologic vomiting can be caused by obstruction of the gastrointestinal tract. On the flip side, vomiting is considered pathologic when it occurs in large volumes, is projectile or has a green or bright yellow color given by bile, or when there are signs of illness, like fever, weight loss, or feeding refusal. 
It usually goes away on its own, but what can also help is feeding the baby in an upright position, burping it frequently during feeding breaks-meaning before switching breasts for breastfeeding moms and every 2 to 3 ounces for bottle-feeding moms-as well as after the baby is done eating, and avoiding active play right after feeds. This is considered normal gastroesophageal reflux, or GER, and generally the vomiting is small-volume, non-projectile or not forceful, formula- or breast milk-colored, and the infant is looking healthy. Causes of vomiting vary a lot depending on the age group of the child, and usually it’s split into newborns or infants that are less than 3 months of age, infants that are over 3 months of age-or children-and adolescents.įirst looking at newborns or young infants, less than 3 months of age, it may be very common to spit up a little bit of milk or formula, usually within the first hour after being fed.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
